
7, 8 Healing time is neither increased nor decreased in closed reduction, but long periods of immobilization may exacerbate stiffness and increase the risk of developing osteopenia. 7 Closed reduction is also commonly used in the treatment of displaced extra-articular fractures by immobilizing the region to limit injury to the soft tissues, tendons, and nerves caused by the displaced bone fragments. Although bone heals naturally, closed reduction can minimize the risk of infection, which is a rare but possible complication using surgical treatment. Nonoperative (nonsurgical) options include immobilization with or without reduction, where the fractured bone is reduced without opening the skin and then subsequently immobilized to avoid potential displacement of fracture while healing. Traditionally, distal radius fractures in those over the age of 65 have been treated both nonsurgically and surgically. 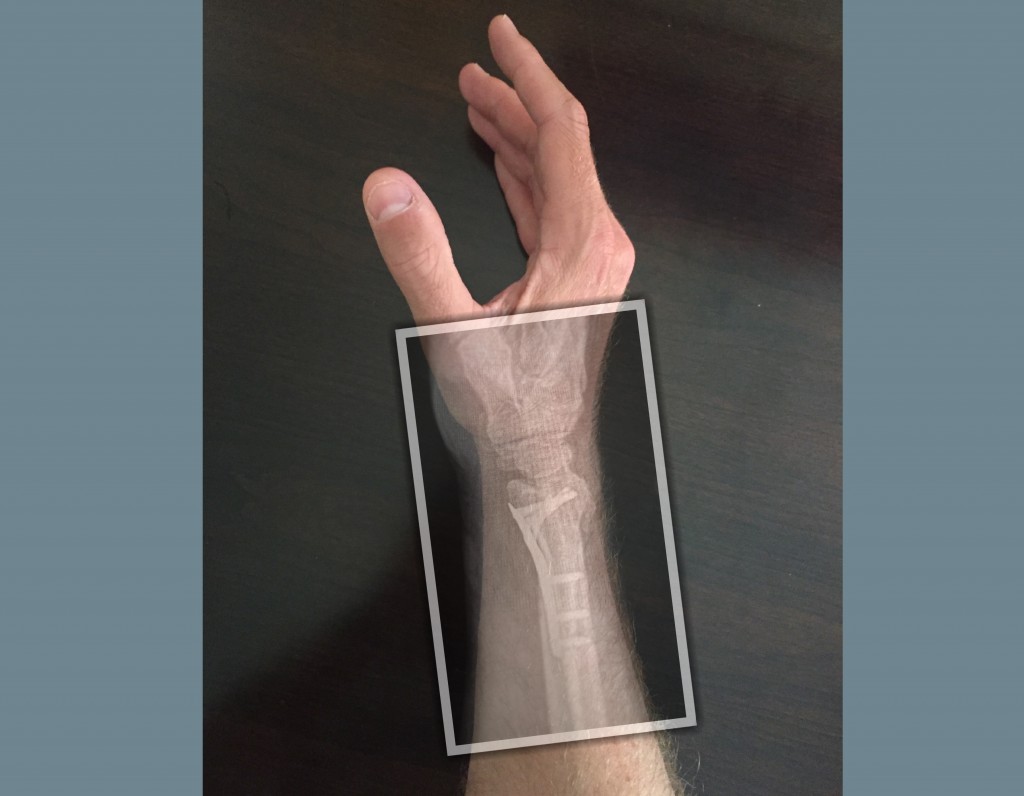
6 Within the same time period, women over the age of 70 have a 60% increased rate of hip fractures. 6 Nellans et al also reported a 5 and 10 times greater rate of vertebral fractures in women and men, respectively, a year after suffering a distal radius fracture. However, mortality rates increased 14% in 7 years following a fracture and men who suffered a distal radius fracture are almost 3 times more likely than women to die during that time period. 6 This number represents all wrist fractures. Nellans et al reported that women who suffered a wrist fracture were 50% more likely to report a functional decline when compared to women without fractures. This number may increase in the future due to the combination of a longer lifespan and low bone density. 5 Distal radius fracture represents 18% of all fractures in patients aged 65 and older, but anatomical reduction in these patients does not correlate with clinical outcome. 5 Moreover, dual-energy X-ray absorptiometry scans revealed higher bone mineral density in men than in women. 4 Conversely, men have less severe fractures than women in part due to the reduced prevalence of osteoporosis. Consequentially, 85% of elderly women exhibit low bone density and 51% have osteoporosis. Age-related fragility is a consequence of accelerated bone breakdown and increases the risk of developing osteopenia and osteoporosis. 3 Postmenopausal women are likely to develop bone-related problems due to decrease in estrogen production, which has been shown to help prevent excessive bone breakdown. 1, 2 The incidence of distal radius fractures increases in women aged 65 and older due to the greater risk of osteoporosis. The aim of this review is to summarize the most common treatments and importance of early referral to hand therapy to improve functional outcomes.ĭistal radius fractures have a high incidence among the aging population and may potentially result in poor functional outcome and impairment. The goal of treatment is to restore mobility, reduce pain, and improve functional outcomes following rehabilitation. However, volar plate fixation is quickly becoming a popular option as it minimizes tendon irritation, reduces immobilization time, and decreases risk of complication. Historically, closed reduction and percutaneous pinning have been the most popular approaches. The nature of the fracture will determine the best treatment option, and surgeons employ a multifactorial treatment approach that includes the patient’s age, nature of injury, joint involvement, and displacement among other factors. Nonsurgical approaches include immobilization with or without reduction, whereas surgical treatments include dorsal spanning bridge plates, percutaneous pinning, external fixation, and volar plate fixation. Traditional approaches to distal radius fractures have included both surgical and nonsurgical treatments, with predominant complaints involving weakness, stiffness, and pain. Although women are more susceptible to hip fractures, men experience a higher mortality rate in the 7 years following a distal radius fracture. Moreover, increased susceptibility to vertebral and hip fractures has been documented in patients a year after suffering a distal radius fracture. GEOPS (Grupo de Estudio de la Osteoporosis)ĭistal radius fractures account for nearly 1 of every 5 fractures in individuals aged 65 or older.Sesiones Clínicas Interhospitalarias Online SOGACOT.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
